
Enhancing "The Basics" of Radiation Oncology Training
R1 Boot Camp (Resident Survivor Series)

Making the transition between intern year and the first year of Radiation Oncology residency can be overwhelming. Every year we provide our residents with an introductory “toolbox” covering some of the basics in the field in order to get their residency training off to a great start. This series is scheduled during the first several weeks after our R1 residents arrive.
Recent topics have included:
- Spinal Cord Compression
- Palliative Lung and SCV Syndrome
- Bone Metastases
- Brain Metastases
- Management of Acute Radiation Toxicities
- “Meet the Treatment Room”
- Treatment Imaging Review
- Intro to Physics
- Intro to Radiation Biology
- Introduction to Simulation and Treatment Delivery
Resident Chart Rounds
The structure of our residency program and the unique learning environment of the Durham VA Hospital allows our residents to lead weekly chart rounds for our veteran patients. This provides a unique learning opportunity – not only to enhance our residents’ knowledge of treatment planning, treatment plan review and on-treatment imaging – but also to review relevant literature in real time. It provides our residents with the opportunity to practice presenting their patients in a chart rounds format so that they are easily able to translate these same skills to their independent practice.
Multi-Institutional Collaborative Radiation Biology Course
We have a longstanding, collaborative radiation biology course that is taught in conjunction with the University of North Carolina (UNC) Radiation Oncology Department. This allows our residents to have access to the world-renown radiation biologists in both departments. This collaborative effort has been so successful that several other institutions have asked to participate, including:
- North Carolina State University
- Upstate Medical University
- Wake Forest University
- The University of Tennessee
ROCC (Radiation Oncology Contouring Competency) Standardized Case Modules
We are in the process of developing a set of case modules for each disease site in order to standardize some of the treatment planning aspects of Radiation Oncology training.
This will permit our graduates to demonstrate competency in treating “bread and butter” cases, utilizing a medium that will allow them to easily translate this competency into the board exam testing environment and independent practice.
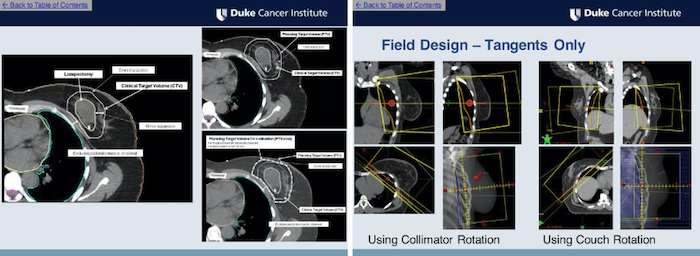
The pilot module for breast cancer treatment has already been developed and outlines the basics of patient simulation, target delineation, beam arrangement, treatment planning and plan evaluation.
GME CLER (Clinical Learning Environment Review) Patient Safety Collaboration
- Quarterly meetings reviewing reported patient safety events in an interprofessional forum (including participation from cancer center leadership) using the “learning from defects” model to improve the safety of patients treated in our department.
- Highlights opportunities for those interested in Quality Improvement (QI) projects.
Coming Soon: Medical Statistics Boot Camp, "Recurrence Rounds"
Anatomy and Simulation Series
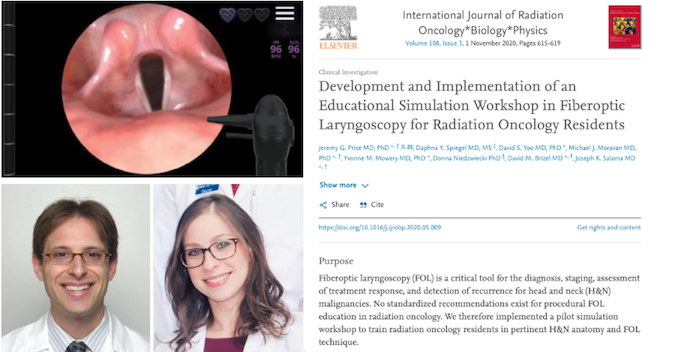
Fiberoptic Laryngoscopy (FOL) Simulation-Based Education
Piloted by former residents Dr. Daphna Spiegel and Dr. Jeremy Price, our residents have the opportunity to participate in a 2-phase simulation workshop in order to introduce them to proper FOL technique.
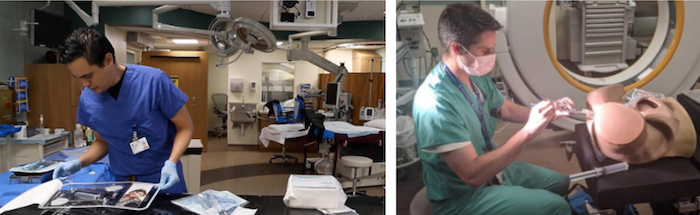
Gynecology Brachytherapy Simulation
- Our residents begin their gynecologic brachytherapy experience by utilizing our pelvic simulator in order to become comfortable manipulating the different applicators for complex brachytherapy delivery (tandem and ovoid, tandem and ring, interstitial needles, etc.).
- We are also working with our physics department to begin 3D-printing various anatomically correct cervixes to allow residents to practice their advanced brachytherapy skills.
Career and Networking Workshops
“Succeed” Seminar Series
Focused on providing residents with information key in making a successful transition from residency to independent practice.
Recent topics have included:
- Chief Residents: Job Hunt Perspectives
- Department Chair: Job Hunt Perspectives
- Financial Planning for Physicians
- Academic Versus Private Practice: Early Career Panel
- Becoming a Successful Clinical Researcher (“The Palta Pathway”)
Resident Coaching Program
Incoming residents are paired with a specific faculty mentor in order to develop a longitudinal relationship focused on providing career advice, networking, etc.
Southeastern Fellows Skills Retreat
We sponsor our R3 residents to attend the Southeastern Fellows Research Skills and Training Workshop every year, which takes place in the town of Duck on the Outer Banks of North Carolina.
Covered topics include:
- How to Give a Successful Presentation
- Transition From Fellow to Faculty
- Grant Applications
- Grant Writing: How to Write Effective Specific Aims
- Families, Careers and Academic Medicine
- Statistics and Trial Design: Asking the Right Questions
- Finding a Mentor
- Leadership for Physician Scientists
- Protocol Development and Management

Radiation Oncology Imaging Program (ROIP)
Visiting professor lecture series highlighting leaders in the fields of radiation biology and advanced imaging.
Recent presenters have included:
- Dr. Peter Glazer (Yale)
- Dr. Salma Jabbour (Rutgers)
- Dr. Bradford Perez (Florida Cancer Specialists & Research Institute)
- Dr. Harvey Mamon (Harvard)
- Dr. Junjie Chen (MD Anderson)
- Dr. Karyn Goodman (Mount Sinai)
- Dr. Kathryn Fowler (UCSD)
- Dr. Simon Powell (MSKCC)
- Dr. Nancy Lee (MSKCC)
- Dr. Ranjit S. Bindra (Yale)
- Dr. Harald Pagnetti (Harvard)
- Dr. Max Diehn (Stanford)
- Dr. Daphne Haas-Kogen (Dana Farber Cancer Institute)
- Dr. Andy Minn (UPenn)
- Dr. Jeanne Nakamura (UCSF)
- Dr. Robert Bristow (University of Toronto)
- Dr. Silvia Formenti (Cornell)
- Dr. Julie Schwarz (Washington University)
Residents spend dedicated time meeting with visiting faculty to discuss their career trajectory, tips for success or other topics (as dictated by resident interests).
Humanism in Medicine
Narrative Oncology Lecture Series
Longitudinal lecture series led by Dr. Brian Quaranta (one of our faculty members who also has a Master’s degree in Shakespeare Studies from the University of Birmingham, United Kingdom) focusing on the humanistic aspects of medicine drawing inspiration from print, film, art and other mediums.
